Cholecalciferol (Vitamin D3)
Cholecalciferol, or vitamin D3, is the form of vitamin D naturally synthesized in human skin upon UVB exposure and is widely supplemented to maintain adequate vitamin D status for bone health and immune function.
Overview
Cholecalciferol, commonly known as vitamin D3, is a secosteroid hormone precursor produced endogenously in the skin through the photochemical conversion of 7-dehydrocholesterol upon exposure to ultraviolet B (UVB) radiation. It is also obtained through dietary sources including fatty fish, egg yolks, and fortified foods. Cholecalciferol is the preferred supplemental form of vitamin D due to its superior efficacy in raising and maintaining serum 25-hydroxyvitamin D levels compared to ergocalciferol (vitamin D2).
Upon ingestion or synthesis, cholecalciferol undergoes two sequential hydroxylation steps: first in the liver to form 25-hydroxyvitamin D (calcidiol), and then in the kidneys to produce the biologically active form, 1,25-dihydroxyvitamin D (calcitriol). Calcitriol functions as a steroid hormone, binding to the vitamin D receptor (VDR) present in virtually every cell type in the body. Its classical role involves regulating calcium and phosphorus homeostasis to maintain skeletal health, but VDR signaling also influences immune cell differentiation, insulin secretion, cardiovascular function, and gene expression in numerous tissues.
Vitamin D deficiency is considered a global public health concern, affecting an estimated one billion people worldwide, particularly those living at higher latitudes, individuals with darker skin pigmentation, older adults, and those with limited sun exposure. Supplementation with cholecalciferol has been extensively studied, with strong evidence supporting its role in preventing rickets, osteomalacia, and falls in elderly populations. Research into its potential benefits for immune function, cancer prevention, cardiovascular health, and mood disorders continues to evolve, with some studies showing promising associations while others yield mixed results depending on baseline vitamin D status and dosing protocols.
Mechanism of Action
Secosteroid Prohormone — Two-Step Bioactivation
Cholecalciferol (vitamin D3) is a secosteroid prohormone synthesized endogenously when UVB radiation (290-315 nm) cleaves the B-ring of 7-dehydrocholesterol in the stratum basale and spinosum of the epidermis. Following hepatic 25-hydroxylation by CYP2R1 (the key vitamin D 25-hydroxylase) to form 25-hydroxyvitamin D3 [25(OH)D3, calcidiol], the circulating prohormone undergoes renal 1-alpha-hydroxylation by CYP27B1 in proximal tubular cells to produce 1,25-dihydroxyvitamin D3 [1,25(OH)2D3, calcitriol] — the hormonally active form. CYP27B1 expression is tightly regulated by PTH (stimulatory), FGF23 (inhibitory), and calcitriol itself (negative feedback) (PMID: 17634462).
Vitamin D Receptor (VDR) — Genomic Signaling
Calcitriol binds the intracellular vitamin D receptor (VDR), a nuclear receptor transcription factor that heterodimerizes with retinoid X receptor (RXR) and binds vitamin D response elements (VDREs) in the promoter regions of over 1,000 target genes. Key genomic targets include TRPV6 and calbindin-D9k (intestinal calcium absorption), RANKL and osteoprotegerin (bone remodeling), cathelicidin (LL-37) and beta-defensin 2 (innate immunity), and p21 and p27 (cell cycle arrest). VDR is expressed in virtually all human tissues, indicating pleiotropic functions far beyond calcium homeostasis (PMID: 16959837).
Calcium & Phosphate Homeostasis
Calcitriol's classical endocrine function is maintaining serum calcium and phosphate within the narrow range required for neuromuscular function and skeletal mineralization. It enhances active transcellular calcium absorption in the duodenum by upregulating TRPV6 calcium channels (apical entry), calbindin-D9k (cytoplasmic shuttling), and PMCA1b calcium ATPase (basolateral extrusion). In bone, calcitriol stimulates osteoblast differentiation via Runx2 expression while modulating RANKL/OPG ratio to regulate osteoclastogenesis (PMID: 21118827).
Immunomodulatory Functions
Calcitriol shifts immune responses from Th1/Th17 toward Th2/Treg polarization by suppressing IL-12, IFN-gamma, and IL-17 production while enhancing IL-10 secretion. In innate immunity, VDR activation in macrophages induces cathelicidin (LL-37) expression, an antimicrobial peptide that disrupts bacterial membranes and neutralizes endotoxin (PMID: 21527855).
Reconstitution Calculator
Reconstitution Calculator
Calculate your peptide dosing

Set up a clean workspace with all supplies ready.
7x / week for weeks
This calculator is provided for informational and educational purposes only. It is not intended as medical advice, diagnosis, or treatment guidance. Always consult a qualified healthcare professional before preparing or administering any substance. PepGuide assumes no liability for decisions made based on these calculations.
Research
Reported Effects
Deficiency Correction:: Effectiveness varies widely by individual; some users require 10,000 IU daily to maintain optimal levels while others respond to 2,000 IU, highlighting the importance of blood testing. Absorption Variability:: Many users struggle with absorption despite supplementation, with genetic factors, magnesium deficiency, and inadequate fat intake commonly cited as limiting factors. Cofactor Requirements:: Users consistently report better results when combining D3 with vitamin K2 (to prevent calcium dysregulation) and magnesium (essential for D3 metabolism). Timing and Context:: Best absorbed when taken with high-fat meals; liquid forms may be more bioavailable than capsules for some individuals
- Effectiveness varies widely by individual; some users require 10,000 IU daily to maintain optimal levels while others respond to 2,000 IU, highlighting the importance of blood testing
- Many users struggle with absorption despite supplementation, with genetic factors, magnesium deficiency, and inadequate fat intake commonly cited as limiting factors
- Users consistently report better results when combining D3 with vitamin K2 (to prevent calcium dysregulation) and magnesium (essential for D3 metabolism)
- Best absorbed when taken with high-fat meals; liquid forms may be more bioavailable than capsules for some individuals
Safety Profile
Common Side Effects
- Nausea, vomiting, and loss of appetite at excessive doses (hypervitaminosis D)
- Constipation or diarrhea
- Weakness, fatigue, and drowsiness
- Metallic taste in the mouth
- Headache and dry mouth
- Elevated blood calcium levels (hypercalcemia) with prolonged high-dose use, which can cause confusion, irregular heartbeat, and kidney damage
Serious Adverse Effects
- Hypercalcemia is the primary toxicity concern, potentially leading to vascular and tissue calcification
- Kidney stones (nephrolithiasis) and kidney damage (nephrocalcinosis) with chronic excessive intake
- Cardiac arrhythmias in severe hypercalcemia cases
- Vitamin D toxicity is rare at doses below 10,000 IU/day but risk increases substantially above this threshold
- Pancreatitis has been reported in cases of severe hypercalcemia
Contraindications
- Hypercalcemia or hypercalciuria (elevated urinary calcium)
- Known hypersensitivity to cholecalciferol or any formulation excipients
- Severe renal impairment without medical supervision
- Granulomatous diseases (sarcoidosis, tuberculosis) where vitamin D metabolism is dysregulated, increasing hypercalcemia risk
- Pre-existing conditions involving calcium dysregulation such as primary hyperparathyroidism
Drug Interactions
- Thiazide diuretics may reduce urinary calcium excretion, increasing the risk of hypercalcemia when combined with vitamin D supplementation
- Corticosteroids can impair vitamin D metabolism and reduce calcium absorption, potentially necessitating higher doses
- Cardiac glycosides (digoxin): hypercalcemia from excessive vitamin D increases the risk of cardiac arrhythmias
- Orlistat, cholestyramine, and other fat-absorption inhibitors may reduce vitamin D absorption
- Anticonvulsants (phenytoin, phenobarbital) accelerate vitamin D catabolism, potentially reducing serum levels
- Concurrent use with calcium supplements requires monitoring to avoid hypercalcemia
Special Populations
- Pregnant and breastfeeding women should not exceed 4,000 IU/day without medical supervision
- Infants and young children require careful dosing to avoid toxicity
- Patients with impaired renal function require dose adjustment and calcium monitoring
- Elderly individuals may have altered vitamin D metabolism and should have periodic serum 25(OH)D level checks
Pharmacokinetic Profile
Cholecalciferol (Vitamin D3) — Pharmacokinetic Curve
SubcutaneousMolecular Structure
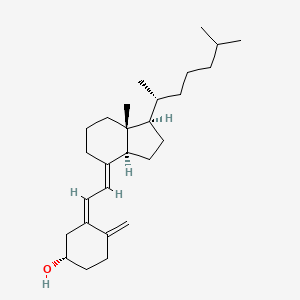
- Formula
- C27H44O
- Weight
- 384.6 Da
- PubChem CID
- 5280795
- Exact Mass
- 384.3392 Da
- LogP
- 7.9
- TPSA
- 20.2 Ų
- H-Bond Donors
- 1
- H-Bond Acceptors
- 1
- Rotatable Bonds
- 6
- Complexity
- 610
Identifiers (SMILES, InChI)
InChI=1S/C27H44O/c1-19(2)8-6-9-21(4)25-15-16-26-22(10-7-17-27(25,26)5)12-13-23-18-24(28)14-11-20(23)3/h12-13,19,21,24-26,28H,3,6-11,14-18H2,1-2,4-5H3/b22-12+,23-13-/t21-,24+,25-,26+,27-/m1/s1
QYSXJUFSXHHAJI-YRZJJWOYSA-NSafety Profile
Common Side Effects
- Sleep Disruption:: Common complaint of worsened sleep quality, insomnia, or restlessness, particularly at higher doses or when taken later in the day
- Anxiety and Overstimulation:: Some users report increased anxiety, mental stimulation, or feelings of being 'wired' from D3 supplementation
- Calcium-Related Issues:: Risk of hypercalcemia with high doses if not balanced with vitamin K2, potentially leading to vascular calcification
- Bone Pain and Discomfort:: Some users experience bone pain, particularly in the legs and femur, which may indicate calcium dysregulation or cofactor imbalances
References (4)
- [3]Vitamin D Resistance as a Possible Cause of Autoimmune Diseases: A Hypothesis Confirmed by a Therapeutic High-Dose Vitamin D Protocol
→ Study proposing that acquired vitamin D resistance contributes to autoimmune disease development and can be effectively treated with high-dose vitamin D3 therapy, with clinical evidence supporting this therapeutic approach.
- [1]Cholecalciferol (vitamin D3): efficacy, safety, and implications in public health
→ Comprehensive review showing vitamin D3 supplementation improves bone mineral density, immune homeostasis, glycemic control, and reduces inflammation, with demonstrated benefits in chronic kidney disease, cystic fibrosis, and inflammatory bowel disease patients.
- [2]Vitamin D for the Prevention of Disease: An Endocrine Society Clinical Practice Guideline
→ Clinical practice guideline evaluating vitamin D's role in disease prevention, providing evidence-based recommendations for supplementation strategies across different populations.
- [4]How Much Vitamin D is Too Much? A Case Report and Review of the Literature
→ Case report and literature review examining vitamin D toxicity thresholds, finding that adverse reactions from supplementation are rare and typically require very high doses over extended periods, with vitamin D levels taking 18 months to normalize after toxicity.
Chlorophyll
Chlorophyll is the green pigment found in plants that enables photosynthesis and is structurally similar to hemoglobin in human blood. As a dietary supplement,
Cholecystokinin (CCK)
**Cholecystokinin (CCK)** is a peptide hormone and neuropeptide originally discovered in 1928 for its ability to contract the gallbladder (Greek: chole = bile,