TRH (Thyrotropin-Releasing Hormone)
Thyrotropin-releasing hormone (TRH, protirelin) is a hypothalamic tripeptide (pGlu-His-Pro-NH2) that stimulates TSH and prolactin release from the anterior pituitary. Beyond the thyroid axis, TRH has documented CNS effects including analeptic, thermoregulatory, and antidepressant-like properties, with research applications spanning depression, spinal cord injury, and consciousness disorders.
Overview
TRH is synthesized as part of a larger 242 amino acid precursor protein (prepro-TRH) that contains six copies of the TRH progenitor sequence Gln-His-Pro-Gly. Post-translational processing by prohormone convertases PC1/3 and PC2 cleaves the precursor, followed by cyclization of the N-terminal glutamine to pyroglutamate and C-terminal amidation of the proline residue by peptidylglycine alpha-amidating monooxygenase (PAM). Both terminal modifications are essential for biological activity — the pyroglutamate protects against aminopeptidase degradation while the C-terminal amide is required for receptor binding.
The primary site of TRH production for thyroid axis regulation is the paraventricular nucleus (PVN) of the hypothalamus, where TRH neurons project to the median eminence and release TRH into the hypothalamic-hypophyseal portal circulation. However, TRH-expressing neurons are found throughout the brain including the raphe nuclei, brainstem reticular formation, hippocampus, amygdala, and spinal cord, consistent with its diverse non-thyroidal functions.
TRH is rapidly degraded in plasma and tissue by pyroglutamyl peptidase II (PPII, also known as TRH-degrading ectoenzyme or TRH-DE), a highly specific zinc metallopeptidase that cleaves the pGlu-His bond. This enzyme is particularly abundant in the anterior pituitary and in brain regions receiving TRH-ergic innervation, serving as a local regulator of TRH bioavailability.
Mechanism of Action
TRH acts through two G protein-coupled receptors: TRH-R1 (widely expressed in pituitary and brain) and TRH-R2 (predominantly CNS, absent from pituitary thyrotropes). Both receptors couple primarily to Gq/11, activating phospholipase C (PLC) to generate inositol 1,4,5-trisphosphate (IP3) and diacylglycerol (DAG). This signaling cascade produces:
- TSH release — IP3-mediated calcium release from endoplasmic reticulum stores and DAG-activated protein kinase C (PKC) stimulate TSH exocytosis from thyrotropes
- Prolactin release — TRH is a potent prolactin secretagogue via the same PLC/IP3/PKC pathway in lactotropes
- Neuronal depolarization — In CNS neurons, TRH closes leak potassium channels, producing membrane depolarization and increased firing rates
- Autonomic activation — Brainstem TRH neurons modulate sympathetic outflow, gastric motility, respiratory drive, and cardiovascular function
The pituitary effects of TRH are modulated by thyroid hormone negative feedback: T3 suppresses TRH receptor expression on thyrotropes and inhibits TRH gene transcription in the PVN, completing the TSH feedback loop. Notably, the prolactin-releasing effect of TRH is not subject to thyroid hormone feedback, which is why TRH administration can produce prolactin elevation even in hyperthyroid states.
Reconstitution Calculator
TRH (Thyrotropin-Releasing Hormone)
Thyrotropin-releasing hormone (TRH) is one of the smallest known bioactive pepti

Set up a clean workspace with all supplies ready.
7x / week for weeks
This calculator is provided for informational and educational purposes only. It is not intended as medical advice, diagnosis, or treatment guidance. Always consult a qualified healthcare professional before preparing or administering any substance. PepGuide assumes no liability for decisions made based on these calculations.
Research
The TRH Stimulation Test
The TRH stimulation test was a cornerstone of thyroid diagnostics for decades. Intravenous administration of 200–500 μg TRH (protirelin) produces a rapid rise in serum TSH within 20–30 minutes in euthyroid individuals. An exaggerated response indicates primary hypothyroidism, an absent response suggests hyperthyroidism or TSH-secreting pituitary adenoma, and a delayed or blunted response may indicate secondary (pituitary) or tertiary (hypothalamic) hypothyroidism.
"The TRH test remains useful in specific clinical scenarios including differentiation of central hypothyroidism subtypes, evaluation of TSH-secreting adenomas, and assessment of the hypothalamic-pituitary-thyroid axis in patients with non-thyroidal illness, although its routine use has been supplanted by ultrasensitive TSH assays." (Hartoft-Nielsen et al., 2004)
TRH and Prolactin Regulation
TRH is the most potent known prolactin-releasing factor, and the TRH-prolactin axis has clinical significance. In primary hypothyroidism, chronically elevated TRH levels can produce hyperprolactinemia, which may cause galactorrhea and menstrual irregularities. This is reversed by thyroid hormone replacement. The TRH-prolactin response is also used diagnostically: an exaggerated prolactin response to TRH may indicate a prolactinoma, while an absent response supports the diagnosis of a non-functioning pituitary adenoma.
TRH in Depression
Multiple lines of evidence implicate TRH in the pathophysiology of depression. Cerebrospinal fluid TRH levels are altered in depressed patients, the TSH response to TRH is blunted in approximately 25% of euthyroid depressed patients, and TRH gene expression in the PVN is increased postmortem in depressed individuals — possibly as a compensatory response.
Direct intrathecal administration of TRH has produced rapid and significant antidepressant effects in small clinical studies. These effects occur within hours, well before any thyroid hormone changes could manifest, confirming that the mechanism is CNS-mediated rather than endocrine.
"Intrathecal administration of TRH produced rapid improvement in depression ratings in treatment-resistant patients, with effects evident within hours of administration. The antidepressant response was independent of changes in thyroid hormone levels, confirming direct CNS-mediated effects." (Marangell et al., 1997)
Spinal Cord Injury Research
TRH and its analogs have been investigated as neuroprotective agents in spinal cord injury (SCI). TRH antagonizes multiple secondary injury cascades including platelet-activating factor (PAF) signaling, lipid peroxidation, and excitotoxicity. In animal models of SCI, TRH administration within the first hours after injury improves neurological outcomes.
"TRH administration after experimental spinal cord injury improves blood flow to the injury site, reduces lipid peroxidation, antagonizes the actions of endogenous opioids and platelet-activating factor, and improves neurological recovery. These effects are mediated by CNS TRH receptors rather than through thyroid hormone changes." (Faden et al., 2005)
The short half-life of TRH (~5 minutes) has motivated the development of metabolically stable analogs. Taltirelin (TA-0910), a TRH analog with improved CNS penetration and a longer half-life, was approved in Japan for spinocerebellar degeneration and has been studied in SCI and other neurological conditions.
Consciousness Disorders
TRH's analeptic properties have led to research in disorders of consciousness, including persistent vegetative state and minimally conscious state following traumatic brain injury. Case reports and small series describe improvement in arousal and awareness following TRH administration, though controlled trials are lacking.
"The neurobiological rationale for TRH in consciousness disorders rests on its ability to increase arousal through multiple brainstem mechanisms, including enhancement of cholinergic and noradrenergic neurotransmission, which are the same pathways disrupted in disorders of consciousness." (Matsumoto et al., 2008)
TRH Analog Development
The rapid enzymatic degradation of TRH by pyroglutamyl peptidase II has driven extensive medicinal chemistry efforts to create metabolically stable analogs with enhanced CNS selectivity:
- Taltirelin (TA-0910) — 10-100x more potent than TRH as a CNS stimulant with longer duration; approved in Japan for spinocerebellar degeneration
- Montirelin (CG-3703) — TRH analog with improved oral bioavailability; studied in impaired consciousness
- RX-77368 — Stabilized TRH analog used extensively in motor neuron disease research
- Midazolam-resistant arousal — Several TRH analogs reverse benzodiazepine-induced sedation in preclinical models
"The development of TRH analogs has focused on improving metabolic stability by modifying the pyroglutamyl residue or the proline amide terminus, which are the sites of enzymatic cleavage. Several analogs achieve 100-fold improvements in half-life while retaining or exceeding the CNS potency of native TRH." (Khomane et al., 2011)
Pyroglutamyl Peptidase II as a Therapeutic Target
Rather than modifying TRH itself, an alternative approach involves inhibiting the degrading enzyme PPII to increase endogenous TRH levels at target sites. PPII is a type II integral membrane protein with its catalytic domain facing the extracellular space, making it accessible to non-cell-permeable inhibitors. Selective PPII inhibitors have shown anxiolytic and antidepressant-like effects in animal models, presumably by potentiating endogenous TRH signaling.
"Inhibition of TRH-degrading ectoenzyme (pyroglutamyl peptidase II) increases endogenous TRH bioavailability in brain regions relevant to mood regulation and produces antidepressant-like effects in behavioral models, representing a novel mechanism-based approach to enhancing TRH neurotransmission." (Charli et al., 2006)
CNS Effects Beyond the Thyroid Axis
TRH produces a remarkable constellation of CNS effects that are entirely independent of thyroid hormone levels. These include:
- Analeptic (arousal) effects — TRH reverses sedation from barbiturates, ethanol, and general anesthetics in animal models
- Antidepressant-like activity — Reduced immobility in forced swim tests; mood improvement in human depression trials
- Thermoregulatory effects — Central TRH administration produces hyperthermia via sympathetic activation
- Respiratory stimulation — TRH increases respiratory rate and tidal volume
- Anticonvulsant activity — Protection against certain seizure models
- Gastric motility — Vagally mediated increases in gastric acid secretion and motility
"TRH is a potent analeptic agent whose central nervous system effects are completely independent of its endocrine actions. The ability of TRH to reverse deep sedation, increase locomotor activity, and raise body temperature appears mediated by brainstem TRH-R1 receptors in the raphe nuclei and reticular formation." (Gary et al., 2003)
Safety Profile
Intravenous protirelin (TRH) for diagnostic testing is generally safe but produces transient side effects in most recipients. Common effects include facial flushing (50%), urge to urinate (40%), nausea (30%), metallic taste (20%), and a brief sensation of warmth or light-headedness. These effects peak within 1–2 minutes and resolve within 5–10 minutes. Transient hypertension can occur, and TRH should be used cautiously in patients with coronary artery disease or seizure disorders. Protirelin has been withdrawn from the US market (though available elsewhere) due to declining clinical use rather than safety concerns.
Pharmacokinetic Profile
TRH (Thyrotropin-Releasing Hormone) — Pharmacokinetic Curve
Intravenous (diagnostic); intranasal, intrathecal (research)Quick Start
- Route
- Intravenous (diagnostic); intranasal, intrathecal (research)
Molecular Structure
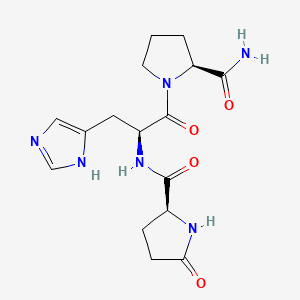
- Formula
- C₁₆H₂₂N₆O₄
- Weight
- 362.38 Da
- CAS
- 24305-27-9
- PubChem CID
- 638678
- Exact Mass
- 362.1703 Da
- LogP
- -2.5
- TPSA
- 150 Ų
- H-Bond Donors
- 4
- H-Bond Acceptors
- 5
- Rotatable Bonds
- 6
- Complexity
- 597
Identifiers (SMILES, InChI)
InChI=1S/C16H22N6O4/c17-14(24)12-2-1-5-22(12)16(26)11(6-9-7-18-8-19-9)21-15(25)10-3-4-13(23)20-10/h7-8,10-12H,1-6H2,(H2,17,24)(H,18,19)(H,20,23)(H,21,25)/t10-,11-,12-/m0/s1
XNSAINXGIQZQOO-SRVKXCTJSA-NResearch Indications
Endocrine
TRH stimulation test distinguishes primary from secondary (pituitary) and tertiary (hypothalamic) hypothyroidism by measuring TSH response. Exaggerated TSH rise indicates primary hypothyroidism; blunted response suggests pituitary dysfunction.
Gold standard for evaluating thyrotroph function and TSH secretory reserve. Used pre- and post-pituitary surgery to assess residual function.
TRH stimulates prolactin release; blunted prolactin response to TRH suggests autonomous prolactin secretion from a prolactinoma.
Neurological
Blunted TSH response to TRH has been observed in approximately 25-30% of patients with major depressive disorder, suggesting hypothalamic-pituitary-thyroid axis dysregulation as a biomarker.
Intravenous TRH and analogs (taltirelin) have shown modest improvement in ataxia symptoms in spinocerebellar degeneration, approved in Japan for this indication.
Limited clinical evidence suggests TRH may have analeptic properties, with case reports of improved consciousness in traumatic brain injury and spinal cord injury patients.
Research Protocols
intravenous Injection
Intravenous administration of 200–500 μg TRH (protirelin) produces a rapid rise in serum TSH within 20–30 minutes in euthyroid individuals. Safety Profile Intravenous protirelin (TRH) for diagnostic testing is generally safe but produces transient side effects in most recipients.
| Goal | Dose | Frequency | Duration |
|---|---|---|---|
| Serum TSH within | 200–500 μg | Per protocol | — |
oral
Administered via oral.
intrathecal Injection
Direct intrathecal administration of TRH has produced rapid and significant antidepressant effects in small clinical studies. "Intrathecal administration of TRH produced rapid improvement in depression ratings in treatment-resistant patients, with effects evident within hours of administration.
intranasal Injection
Administered via intranasal.
Interactions
Peptide Interactions
Chronic administration of levodopa inhibits the TSH response to TRH. Patients on levodopa therapy may show blunted pituitary response to TRH stimulation, reducing its diagnostic and therapeutic utility. Source: Drugs.com TRH prescribing information; DrugBank DB09421.
What to Expect
What to Expect
Rapid onset expected; half-life of ~5–6 minutes (plasma) indicates fast-acting pharmacokinetics
These effects peak within 1–2 minutes and resolve within 5–10 minutes.
Due to short half-life (~5–6 minutes (plasma)), effects are expected per-dose; consistent daily administration maintains therapeutic levels
Regular administration schedule required; effects are dose-dependent and do not persist between doses
Safety Profile
Common Side Effects
- Thyroid Dysregulation:: Improper use could potentially affect thyroid hormone balance
- Pituitary Effects:: May influence prolactin secretion and other pituitary functions
- Individual Variation:: Effects likely vary significantly based on existing thyroid status
- Limited User Reports:: Minimal consumer-level side effect data due to restricted availability
Quality Indicators
What to look for
- Well-established safety profile
- Multiple peer-reviewed studies available
Caution
- Short half-life may require frequent dosing
Frequently Asked Questions
References (16)
- [11]Matsumoto A et al TRH in disorders of consciousness Brain Inj (2008)
- [13]Charli JL et al TRH-degrading ectoenzyme: functional implications Peptides (2006)
- [8]
- [10]
- [16]Sun Y et al TRH receptors: pharmacology and CNS function Pharmacol Ther (2009)
- [9]Marangell LB et al Effects of intrathecal thyrotropin-releasing hormone (protirelin) in refractory depressed patients Arch Gen Psychiatry (1997)
- [12]Khomane KS et al Novel thyrotropin-releasing hormone analogs: a patent review Expert Opin Ther Pat (2011)
- [14]Boler J et al The identity of chemical and hormonal properties of the thyrotropin releasing hormone and pyroglutamyl-histidyl-proline amide Biochem Biophys Res Commun (1969)
- [15]Lechan RM, Fekete C The TRH neuron: a hypothalamic integrator of energy metabolism Prog Brain Res (2006)
- [7]Hartoft-Nielsen ML et al The TRH test in the diagnosis of hypothalamic-pituitary disorders Eur J Endocrinol (2004)
- [1]The Link between Thyroid Function and Depression
→ Reviews the relationship between thyroid function and depression, noting that thyroid hormone supplements appear to accelerate and enhance clinical response to antidepressant drugs, and that various thyroid abnormalities including blunted TSH response to TRH are commonly documented in depression.
- [2]Rapid modulation of TRH-like peptides in rat brain by thyroid hormones
→ Demonstrates that TRH and TRH-like peptides in brain regions involved in mood regulation respond rapidly to thyroid hormone changes within 2 hours, suggesting non-genomic mechanisms may contribute to psychiatric effects of thyroid disease and thyroid hormone treatment for depression.
- [3]TRH Action Is Impaired in Pituitaries of Male IGSF1-Deficient Mice
→ Studies loss-of-function mutations in IGSF1 gene that cause central hypothyroidism, examining how TRH action is affected in thyrotrope cells and the mechanisms underlying TSH production.
- [4]A novel TRH-PFTAIRE protein kinase 1 pathway in the cerebellum
→ Identifies a molecular pathway showing TRH regulates PFTAIRE protein kinase 1 (PFTK1) in the cerebellum in a dose-dependent manner, providing insights into TRH's neurophysiological actions in the brain beyond thyroid regulation.
- [5]Cyclo(His-Pro) Exerts Protective Carbonyl Quenching Effects through Its Open Histidine Containing Dipeptides
→ Examines cyclo(His-Pro), a cyclic dipeptide found in protein-rich foods with favorable pharmacokinetic properties and various biological activities, including antioxidant and protective effects through its open dipeptide forms.
- [6]Thyrotropin-releasing hormone gene expression in the anterior pituitary: Stimulation by glucocorticoids
→ Shows that glucocorticoids substantially stimulate TRH gene expression and cellular TRH accumulation in cultured anterior pituitary cells, revealing hormonal regulation of TRH production.
TREMELLA
Tremella fuciformis, also known as white jelly mushroom or snow fungus, is an edible medicinal mushroom traditionally used in Asian medicine. Its primary bioact
TRIBULUS TERRESTRIS
Tribulus terrestris is a plant from the Zygophyllaceae family containing bioactive compounds including steroidal saponins, flavonoids, and alkaloids. It is trad