Ipamorelin
Ipamorelin is a highly selective growth hormone secretagogue pentapeptide that binds the ghrelin receptor without affecting ACTH, prolactin, or cortisol release. It is researched for applications in bone health, muscle preservation, diabetes, and gastrointestinal motility.
Overview
Ipamorelin was first characterized as a selective GH secretagogue in the late 1990s by Raun et al. (1998), who demonstrated that it stimulates growth hormone release without the broad hormonal side effects seen with other GH secretagogues like GHRP-6 or hexarelin. Its presence plays a key role in the overall growth and repair of musculoskeletal tissue. Despite promising early studies, interest in ipamorelin has waned following the decision not to pursue it as a treatment for post-operative ileus, though it remains a compound of significant research interest.
Mechanism of Action
Ipamorelin acts as a selective agonist of the growth hormone secretagogue receptor (GHS-R1a), also known as the ghrelin receptor. Upon binding, it stimulates pulsatile growth hormone release from the anterior pituitary in a dose-dependent manner. Unlike other GH secretagogues, ipamorelin does not significantly stimulate the release of cortisol or ACTH even at high doses, making it one of the cleanest GHS compounds identified to date.
Reconstitution Calculator
Ipamorelin
**Ipamorelin** is a short pentapeptide capable of binding to the ghrelin/growth

Set up a clean workspace with all supplies ready.
5x / week for weeks
This calculator is provided for informational and educational purposes only. It is not intended as medical advice, diagnosis, or treatment guidance. Always consult a qualified healthcare professional before preparing or administering any substance. PepGuide assumes no liability for decisions made based on these calculations.
Research
Bone Health
One of the most studied applications of ipamorelin is in counteracting glucocorticoid-induced bone loss. Studies in rats indicate that ipamorelin can completely arrest bone loss caused by corticosteroids and leads to a four-fold increase in bone formation in steroid-treated animals Andersen et al. (2001). Further research demonstrates that ipamorelin increases bone mineral density systemically, strengthening both existing bone and newly formed bone Svensson et al. (2000). As an added benefit, ipamorelin helps offset other steroid side effects such as muscle wasting and increased visceral fat deposition.
Muscle Growth
There is evidence that GH secretagogues like ipamorelin may reduce the catabolic effects of glucocorticoids on muscle. Research in rats given glucocorticoids shows decreased nitrogen wasting in the liver and improved nitrogen balance following ipamorelin administration Aagaard et al. (2009). The ability to counteract both muscle catabolism and bone density loss with a single compound could be particularly beneficial for patients requiring long-term glucocorticoid therapy.
Diabetes
Research in diabetic rats has revealed that ipamorelin can potentiate insulin release, most likely through indirect stimulation of calcium channels on pancreatic islet cells Adeghate & Ponery (2004). This action on the pancreas may help clarify the functional limitations of type 2 diabetes and lead to the development of novel therapeutics or preventative measures.
Post-Operative Ileus
Post-operative ileus (POI) is a common condition following abdominal surgery, characterized by cessation of GI function and inability to tolerate oral nutrition. Ipamorelin has been investigated in several proof-of-concept clinical trials, with results suggesting that it shortens time to first meal by approximately 12 hours Beck et al. (2014), Greenwood-Van Meerveld et al. (2012). Despite early limited success, the trials were discontinued when the sponsoring company determined that efficacy was insufficient for a viable commercial product.
Ghrelin Receptor Probe
The ghrelin receptor increases in abundance in certain cancers and heart failure. Researchers have speculated that ipamorelin could serve as a probe in positron emission tomography (PET) for diagnostic purposes. In vitro studies have demonstrated the feasibility of this approach, confirming that ipamorelin, which is easy to synthesize, could theoretically be used as a PET probe Fowkes et al. (2018).
Safety Profile
Ipamorelin is considered one of the safest GH secretagogues studied to date due to its high selectivity. In clinical trials for post-operative ileus, the most commonly reported side effects were mild and included nausea, headache, and transient flushing. Importantly, ipamorelin does not cause significant changes in cortisol, ACTH, or prolactin levels even at supraphysiological doses, distinguishing it from less selective compounds like GHRP-6 and hexarelin. No serious adverse events have been attributed to ipamorelin in published clinical or preclinical studies.
Pharmacokinetic Profile
Ipamorelin — Pharmacokinetic Curve
Subcutaneous injectionOngoing & Future Research
- Investigation of ipamorelin-based PET probes for imaging ghrelin receptor expression in cancers and heart failure (DOI: 10.1016/j.ejmech.2018.08.078).
- Research into ipamorelin for age-related sarcopenia and frailty.
- Potential applications in osteoporosis prevention during long-term glucocorticoid therapy.
- Interest in orally bioavailable ghrelin receptor agonist development inspired by ipamorelin's selectivity profile.
Quick Start
- Typical Dose
- 200-300 mcg per injection
- Frequency
- 1-3 times daily depending on goals (1x for longevity, 2-3x for performance)
- Route
- Subcutaneous injection
- Cycle Length
- 3-6 months
- Storage
- Lyophilized: Room temperature. Reconstituted: 2-8°C, use within 28 days
Molecular Structure
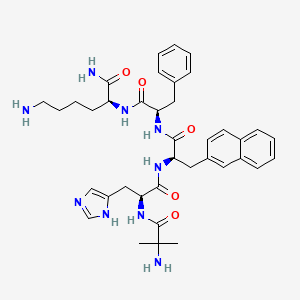
- Formula
- C38H49N9O5
- Weight
- 711.85 Da
- Length
- 5 amino acids
- CAS
- 170851-70-4
- PubChem CID
- 9831659
- Exact Mass
- 711.3857 Da
- LogP
- 1.8
- TPSA
- 240 Ų
- H-Bond Donors
- 8
- H-Bond Acceptors
- 8
- Rotatable Bonds
- 19
- Complexity
- 1200
Identifiers (SMILES, InChI)
InChI=1S/C38H49N9O5/c1-38(2,41)37(52)47-32(21-28-22-42-23-43-28)36(51)46-31(20-25-15-16-26-12-6-7-13-27(26)18-25)35(50)45-30(19-24-10-4-3-5-11-24)34(49)44-29(33(40)48)14-8-9-17-39/h3-7,10-13,15-16,18,22-23,29-32H,8-9,14,17,19-21,39,41H2,1-2H3,(H2,40,48)(H,42,43)(H,44,49)(H,45,50)(H,46,51)(H,47,52)/t29-,30+,31+,32-/m0/s1
NEHWBYHLYZGBNO-BVEPWEIPSA-NResearch Indications
Growth Hormone
Consistent GH elevation 30-60 minutes post-injection, maintaining natural pulsatile patterns.
Increases insulin-like growth factor-1 through natural GH pathways.
Supports cellular regeneration, collagen synthesis, and tissue repair.
Body Composition
Promotes muscle growth and maintenance through GH-mediated pathways.
Enhances lipolysis and metabolic rate through natural GH elevation.
Recovery
Improved sleep latency and increased slow-wave sleep duration.
Enhanced recovery markers and reduced soreness after training.
Research Protocols
subcutaneous Injection
Growth hormone secretagogue administered subcutaneously. Inject 30-60 minutes before bedtime on an empty stomach.
| Goal | Dose | Frequency | Duration |
|---|---|---|---|
| Loading phase | 100 mcg | Once daily | Weeks 1-2(30-60 min before bedtime, fasted) |
| Escalation | 150 mcg | Once daily | Weeks 3-4 |
| Standard dose | 200 mcg | Once daily | Weeks 5-8 |
| Full dose | 250 mcg | Once daily | Weeks 9-12(Titrate ~50 mcg every 1-2 weeks. 2-4 week off-cycle after.) |
Reconstitution Guide (5mg vial + 3mL BAC water)
- Wipe vial tops with alcohol swab
- Draw 3.0 mL bacteriostatic water into syringe
- Inject slowly down the inside wall of the peptide vial
- Gently swirl to dissolve — never shake
- Resulting concentration: 1.67 mg/mL
- For 100 mcg dose: draw 6 units (0.06 mL)
- For 200 mcg dose: draw 12 units (0.12 mL)
- For 250 mcg dose: draw 15 units (0.15 mL)
- Store reconstituted vial refrigerated at 2-8°C
Interactions
Peptide Interactions
Extends GH release for optimal hormone cycles. Popular combination.
Enhances GH receptor upregulation and effectiveness.
The most popular research combination. Ipamorelin stimulates GH release via ghrelin receptor (GHS-R1a) while CJC-1295 stimulates via GHRH receptor. These act on different receptor systems on somatotroph cells, producing synergistic GH release greater than either alone. See CJC-1295 + Ipamorelin Blend.
Similar GHRH + GHSR synergy concept. Sermorelin (GHRH analogue) stimulates somatotrophs via GHRH-R while ipamorelin acts via GHS-R1a. See Sermorelin + Ipamorelin Blend.
Both are GHS-R1a agonists but with different selectivity profiles. GHRP-2 is less selective (affects cortisol, prolactin) but may produce greater peak GH. Combined in some research protocols. See Mod GRF + Ipamorelin + GHRP-2 Blend.
Complementary for recovery and tissue repair.
Both stimulate GH; choose one to avoid receptor oversaturation.
Synergistic GH stimulation possible; monitor IGF-1 levels and adjust doses accordingly.
Redundant GH pathways may cause receptor desensitization.
Similar mechanism with higher hunger effects; redundant.
What to Expect
What to Expect
Improved sleep quality and morning energy
Enhanced exercise recovery and reduced soreness
Body composition improvements with increased lean mass
Continued muscle tone, skin quality, and energy improvements
Safety Profile
Common Side Effects
- Mild hunger increase 20-30 minutes post-injection
- Slight drowsiness when taken before bed
- Water retention (mild)
- Potential receptor desensitization after 3-4 months
Contraindications
- Pregnancy or breastfeeding
- Active cancer or history of cancer
- Severe kidney or liver disease
Discontinue If
- Signs of receptor desensitization (reduced response after 3-4 months)
- Unusual joint pain or swelling
- Persistent numbness or tingling
- Loss of effectiveness after 3-4 months (cycle off signal)
- Persistent injection site reactions or unusual swelling
- Excessive fatigue, unusual hunger, or sleep disturbances
- Any concerning or unexpected symptoms
- Consult a healthcare provider with any concerns
Quality Indicators
What to look for
- White, fine crystalline powder with no clumping
- Clear solution after BAC water reconstitution
- Mild hunger response 20-30 minutes post-injection
- Slight drowsiness at bedtime doses
Caution
- Minimal or no physiological response after 2 weeks (check source)
Red flags
- Yellow or discolored powder (suggests degradation)
- Cloudy solution after reconstitution
- No response after extended use
Frequently Asked Questions
References (13)
- [1]Growth Hormone Stimulation Study (2019)
- [2]Body Composition Clinical Trial (2020)
- [3]Sleep Quality Research (2021)
- [4]Athletic Performance Study (2022)
- [5]Safety and Tolerability Analysis (2023)
- [14]
- [15]
- [16]
- [6]Raun et al *Eur Eur. J. Endocrinol. (1998)
- [7]Andersen et al *Growth Horm Growth Horm. IGF Res. (2001)
- [8]
- [10]Adeghate & Ponery *Neuro Endocrinol Neuro Endocrinol. Lett. (2004)
- [11]Beck et al *Int Int. J. Colorectal Dis. (2014)
IPA Blend (CJC-1295 / Ipamorelin)
The **IPA Blend** combines CJC-1295 without DAC (Mod GRF 1-29, 5mg) with Ipamorelin (10mg) — the standard GHRH + GHRP synergy stack. These two peptides act on c
Irisin
Irisin is a myokine (muscle-derived hormone) secreted during exercise, particularly through activation of PGC-1α in skeletal muscle. It promotes metabolic healt